How Can We Use AI to Improve the Diagnosis of Tuberculosis?
There's a growing number of patients with tuberculosis and the number of radiologists for its diagnosis isn't following. We will soon need AI for triaging and screening, especially in countries with lower socio-economic status.
Tuberculosis (TB) is an infectious disease caused predominantly by the bacteria Mycobacterium tuberculosis. It usually affects the lungs and is characterised by the formation of granulomas where the disease is present. About 10 million people fall ill with TB every year, and 1.4 million people died of it in 2019. This makes it one of the top 10 causes of death and the leading cause of death from a single infectious agent (more here). Though not intuitive, digital health is also slowly making its way into tuberculosis.
There are three interesting papers I discovered about this topic. Let’s first look at the diagnostic accuracy of deep learning in medical imaging.
For now, a human radiologist interprets each medical image. But because of a growing number of patients, radiology will soon need the help of AI. This is especially true for low-to-middle-income countries, which are experiencing the biggest demand for radiologists. Deep learning (DL) as a subfield of AI can address this problem.
When looking at the results across different studies, we can notice that DL algorithms in general have a clinically acceptable diagnostic accuracy in identifying the disease. The problem is that this is just an estimate, which is uncertain due to high heterogeneity and variance of patients and data.
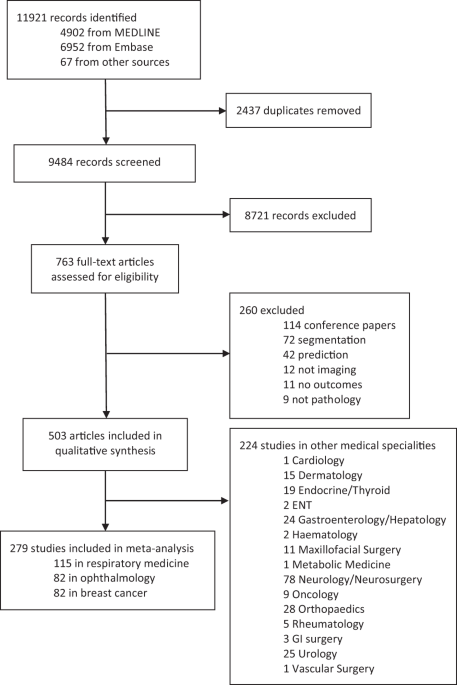
An important number I intentionally left out in the beginning is that only 7.1 million cases (of 10 million) were included in tuberculosis programmes. We can agree that there’s a diagnostic gap in tuberculosis. The second study addressed whether AI technologies could bridge this gap. Interestingly, some analysed AI algorithms achieved higher specificity (90%) than human radiologists. However, the algorithms performed worse in people over 60 years with a history of tuberculosis. Nonetheless, The World Health Organization even recommended the use of computers in triage and screening of tuberculosis instead of radiologists in patients older than 15 years.
Screening for tuberculosis using AI could bridge the diagnostic gap. Although rapid molecular tests are available, they’re too expensive for population-wide screening. This is resource-intensive in every aspect, but using chest radiographs and AI is still more accessible than testing. Additionally, it offers two key advantages:
- It’s possible to detect subclinical and asymptomatic patients. More than half of patients are asymptomatic, but still detectable on chest radiographs.
- It’s less expensive to scale it and thus theoretically more accessible in lower socioeconomic countries. This is also exactly where the need for radiologists is the biggest, which could be decreased with screening.

These same algorithms were used to triage patients in rural South Africa, which is what the third study was about. This was not exactly screening for the disease because the chest radiograph was used only to refer patients for sputum collection. But perhaps this is the best of both worlds. Theoretically, we could first use an algorithm to determine which patients need further diagnostics and then confirm the diagnosis with molecular tests. Such studies could also be a great basis for further exploration and the possibility of screening.
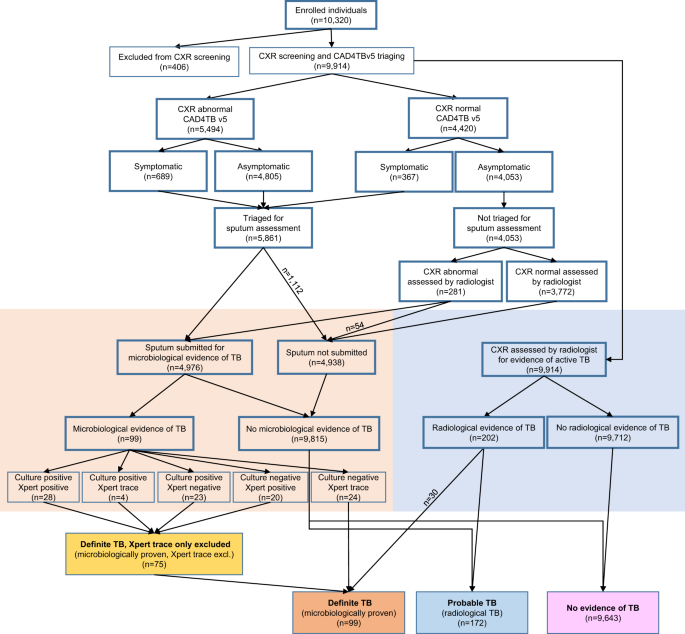
There are certainly not many studies on this matter, but it’s great to see how technology can potentially bridge two gaps. The first one is diagnostic, and the second one is socioeconomic. But for some reason, we predominantly only discuss digital solutions in countries with advanced healthcare systems. The true need, however, might be where people don’t have access to proper diagnostics.





